INTRODUCTION
Ossification of the posterior longitudinal ligament (OPLL) is commonly reported in Asian populations21). OPLL may involve the cervical and thoracic spine and could cause severe myelopathy5). Conservative treatment is ineffective to treat thoracic myelopathy. Despite several surgical techniques that have been reported for treatment of thoracic OPLL, satisfactory results are not always achieved. Thus far, there are no standard treatment protocols established for thoracic OPLL4). Direct removal of the massive OPLL is the most valid method of relieving anterior spinal cord compression10,19,22,24). However, in anterior decompression, the compressed spinal cord is quite vulnerable to injury during removal of OPLL23). Postoperative neurological deterioration and complications have been reported in several articles3,15). In conventional anterior decompression and fusion, the patients were confined to bed for 3 weeks3). Anterior instrumentation might be needed to maintain stability. A hard orthosis was used postoperatively3). In this technical note, we present two cases using our novel technique to remove OPLL, which is a relatively safe and minimally invasive procedure.
ILLUSTRATIVE CASE 1
History
This 51-year-old female was referred to our hospital with right lower limb radiating pain and paresis. Sphincter tone had decreased. Her symptoms had gradually progressed over the previous 2 months. Thoracic OPLL at T6-7 had been identified at our hospital, and conservative treatment had been tried without success. Her medical history included hypertension.
Examination
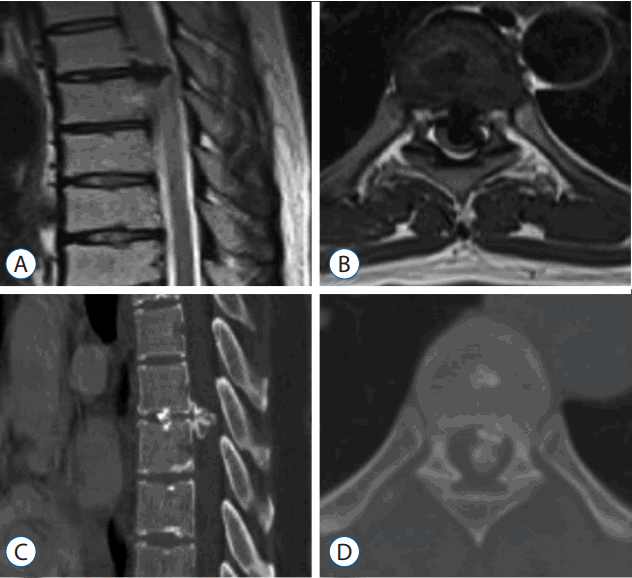
After admission to our hospital, the patient complained of difficulty walking with bilateral lower extremity weakness. She depended on a wheelchair. Physical examination revealed hyperreflexia at the bilateral knee and ankle joints. As a measure of thoracic myelopathy, her preoperative Japanese Orthopedic Association (JOA) score was 9 (total score of 17). Myelography, computed tomography (CT) scanning, and magnetic resonance imaging (MRI) revealed an isolated huge beak-type OPLL at the T6-7 level with severe spinal cord compression (Fig. 1) and mild C4-5 spinal stenosis.
Postoperative course
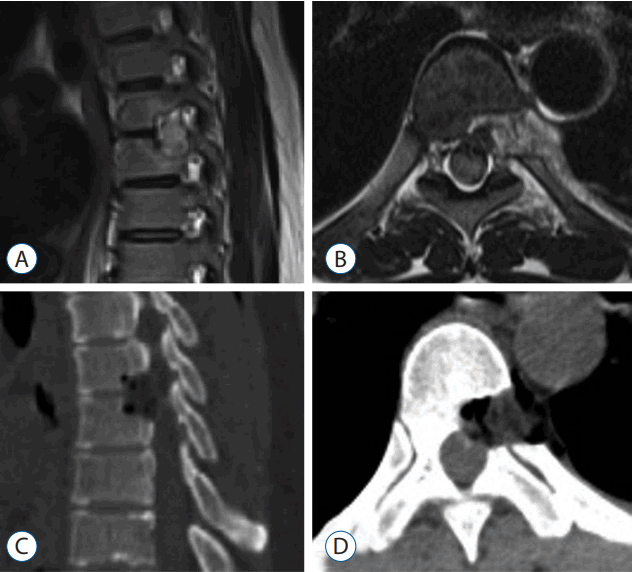
After the operation, the patientŌĆÖs preoperative neurological symptoms gradually improved. No spinal orthosis was used. One week after surgery, the patient could walk using a cane. Postoperative CT and MRI revealed complete removal of the OPLL (Fig. 2). After 6 months, the patientŌĆÖs preoperative neurological symptoms had improved. His postoperative JOA score was 14 (total score of 17).
ILLUSTRATIVE CASE 2
History
This 54-year-old female with a 6-month history of progressive gait disturbance and bilateral lower extremity radiating pain (right>left) was admitted to our institute. She also had hypoesthesia in both lower legs. Her symptoms had been gradually progressing.
Examination
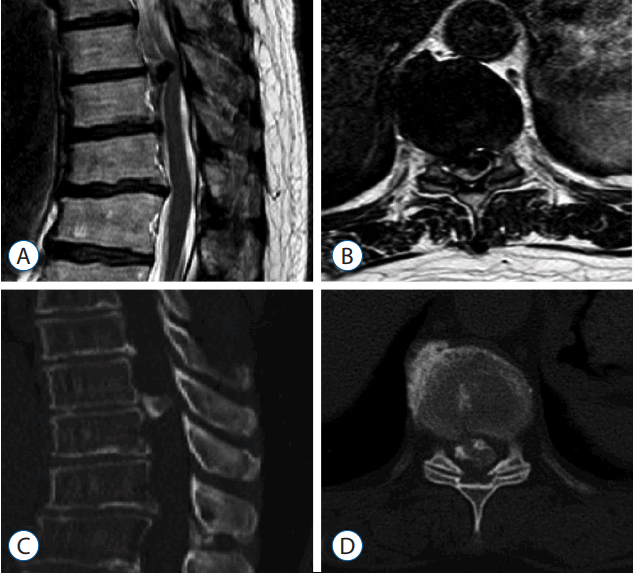
A manual muscle test revealed a tibialis anterior score of 5/5 in right side, 2/5 in left side and an extensor hallucis longus score of 5/5 in right side, 2/5 in left side, particularly in the ankle dorsiflexors because of a past left ankle fracture. As a measure of thoracic myelopathy, her preoperative JOA score was 10 (total score of 17). CT scans showed massive OPLL at the T9-10 level. MRI of the thoracolumbar spine demonstrated ventral bony masses with severe anterior compression of the spinal cord at the same level (Fig. 3).
Postoperative course
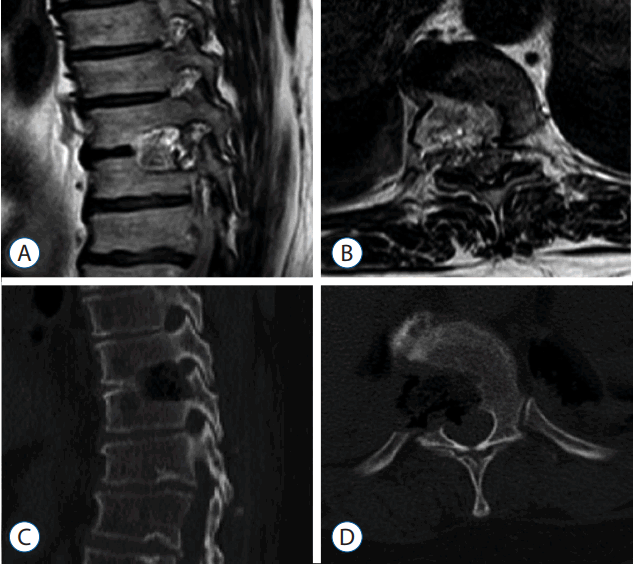
Immediately after surgery, this patientŌĆÖs preoperative lower extremity radiating pain had improved. Ten days after the operation, the patient could walk using a cane. Postoperative CT and MRI revealed total removal of the OPLL (Fig. 4). After 4 months, her preoperative gait disturbance had improved, and she could walk without a cane. Her postoperative JOA score was 14 (total score of 17).
Surgical technique
Because of massive OPLL with spinal cord compression and a kyphotic thoracic spine, posterior laminectomy or laminoplasty might not provide enough decompressive effect. Anterior decompression via a posterior approach was very difficult because of inaccessibility to the surgical field of view. Therefore, we decided to perform a minimally invasive anterior decompression technique without instrumented fusion via transthoracotomy for thoracic OPLL under intraoperative monitoring using motor evoked potentials and somatosensory evoked potentials.
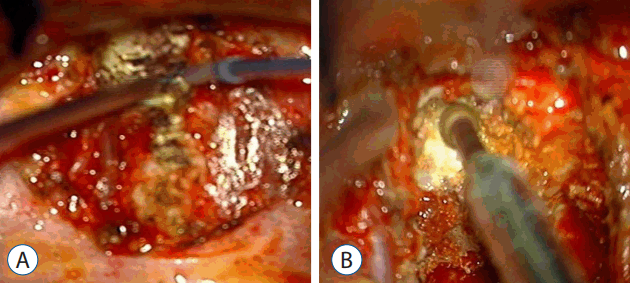
The patients were placed in the decubitus position with the dominant side of the OPLL up. An anterior lateral approach via thoracotomy was used. The index disc was exposed and confirmed by fluoroscopy. The rib head was excised, and the pedicle below the index level was exposed (Fig. 5A).
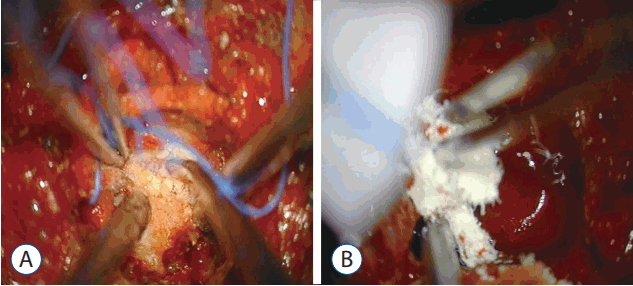
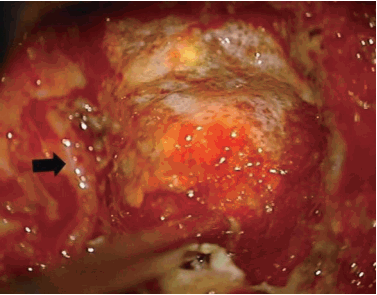
Two pedicles (upper and lower body) and the posterior margin of the disc were identified under a microscope. The posterior half of the disc was removed. Additionally, ostectomy was simultaneously performed with a high speed burr. The area included the partial posterior vertebral body of the inferior upper vertebra, superior lower vertebra, and total portion of the pedicle in the lower vertebra. The partial vertebral body ostectomy provided space for the ventral side of OPLL. The pedicle ostectomy (Fig. 5B) provided more space to deal with the adhesion between the OPLL and the dura. Via this space, the OPLL and the dural sac could be seen directly. The OPLL mass was floated by drilling delicately. After releasing the adhesion between the ossified ligament and the ventral aspect of the dural sac, the OPLL was removed completely (Fig. 6A). Avitene and cottonoids were used for bleeding control between the OPLL mass and the dural sac (Fig. 6B). During the operation, the upper and lower segmental arteries were preserved, and the nerve root was always protected through the whole procedure (Fig. 7). Unfortunately, there was a dural tear and cerebrospinal fluid (CSF) leakage in the 2nd case, so a Lyoplant patch was inserted in the subdural area followed by Tachosil patch application. The chest tube was kept in the operating room after the operation. After 2 weeks drainage, drainage was reduced and CSF leakage was not observed. And then, chest tube was removed.
RESULTS
We used this surgical method in 2 patients with a huge beaked-type OPLL in the thoracic level. Complete removal of the OPLL via anterior decompression without instrumented fusion was accomplished. The 1st case had no intraoperative or postoperative complications, and the 2nd case had 1 intraoperative complication (dural tear) and no postoperative complications. There were no residual symptoms of the lower extremities.
DISCUSSION
Decompression surgery is the treatment of choice for compressive myelopathy2). However, the surgical outcomes of thoracic OPLL are not as favorable compared with those of cervical OPLL12). The unfavorable outcome can be explained by anatomical and pathophysiological factors of thoracic OPLL: 1) the natural kyphosis of the thoracic spine may limit the positive effect of posterior decompression; 2) the thoracic spinal cord is relatively avascular, which is more vulnerable during decompressive manipulation11); and 3) the anterior approach is restricted and the technique is demanding. The strong adhesion between OPLL and the dural sac increases the difficulty of removing the OPLL and increases the risk of intraoperative damage. Factors that significantly contributed to surgical outcomes were the combined use of instrumentation and the level of maximum OPLL at the thoracic spine12). Surgical complications can occur early or be delayed. The perioperative complications reported by surgeons include epidural hematoma, CSF leakage, infection, and neurological deterioration15). The real causes of early neurological deterioration are not well known.
The surgical management of thoracic OPLL is challenging, even for experienced surgeons. Surgical management for OPLL includes several options: 1) posterior decompression with or without instrumentation; 2) laminoplasty; 3) posterior decompression with instrumented fusion then 2nd stage anterior decompression; 4) anterior decompression via a posterior approach; and 5) anterior decompression via an anterior approach. A multiple institutional retrospective study has been performed including 34 hospitals in which detailed data was analyzed on patients who had thoracic OPLL8). The study analyzed the following procedures: beak-type OPLL treated by anterior decompression with instrumented fusion using an anterior approach and laminoplasty; continuous waveform and cylindrical type OPLL treated by laminoplasty; and mixed type OPLL treated by laminectomy with fusion and anterior decompression with fusion via an anterior approach. The results revealed no statistically significant difference in outcomes among the different surgical methods.
Because of lordotic or mild kyphotic curvature at the upper thoracic spine, indirect posterior decompression can be accomplished by laminectomy or extensive laminoplasty12). Although the thoracic spine anchored to the chest cage has limited motion, progressive kyphosis might occur after posterior laminectomy. Some surgeons use posterior segmental instrumentation with fusion for correction of kyphosis or prevention of kyphosis progression. Thus, the posterior decompressive effect can be maintained23). However, favorable outcomes may not be achieved because the OPLL remains and because of the physiological kyphosis of the thoracic spine14,20). The spinal cord has limited dorsal shift in the middle and lower thoracic spine.
Some authors advocate favorable surgical outcomes using the circumferential approach for complete decompression7,19). This approach improves neurological function better than posterior laminectomy alone18). Matsuyama et al. showed that kyphotic reduction in the thoracic spine provides a dorsal shift of the spinal cord by using intraoperative sonography8,14). Posterior decompression may provide posterior space for the spinal cord to escape from injury by anterior manipulation19). Therefore, the advantage of this surgical method was a relatively low risk of spinal cord damage while removing the OPLL via an anterior approach. Tomita et al.19) reported staged circumspinal decompression including a posterior decompression followed by anterior decompression via thoracotomy. They suggested deep gutter drilling in the bilateral vertebral bodies after posterior laminectomy. Then thoracotomy for anterior decompression with partial vertebrectomy, discectomy, removal of OPLL, and interbody fusion were performed. However, there is still the possibility of spinal cord injury in cases of OPLL with extensive involvement in the thoracic spine. The circumspinal approach has not become the standard protocol for thoracic OPLL because combined operation can increase the operation time, surgical stress, technical demands, and anesthesia risk.
Direct removal of the OPLL is the optimal objective of the surgery. Some surgeons have reported relatively favorable surgical outcomes using anterior decompression via a posterior approach1,17). However, Takahata et al.18) reported a relatively high rate of complications, including neurological deterioration in 33% and dural tear in 40% of the patients. Adherence of the OPLL to the ventral side of the dura increases the risk of spinal cord injury and removal difficulty. It was supposed that the complications were related to insufficient space and the operative field of view. Anterior decompression via a posterior approach has several disadvantages: 1) increasing the risk of spinal cord ischemia because the thoracic nerve roots were ligated16) and 2) a larger operative wound and surgical stress7). However, the OPLL was too massive in this case. Anterior decompression via a posterior approach was very difficult due to the inaccessibility of the surgical field.
Anterior decompression via the transthoracic approach is the most logical approach in the treatment of thoracic myelopathy caused by thoracic OPLL3). However, there are relatively high risks of perioperative complications6,23). Postoperative neurological deterioration was reported in several publications3,15). The patients were restricted to bed and equipped with spinal orthosis after operation. Our technique of minimally invasive anterior decompression without instrumented fusion is a modification of the conventional operation. This surgical method has several advantages: 1) it retains the advantages of the conventional anterior approach (for example, visualization of the OPLL and anterolateral side of the dural sac directly and a small operative wound); 2) it provides a wider view at the anterior lateral side of the dural sac to maneuver in the anterior decompression than the posterior approach; 3) no nerve roots were sacrificed; 4) neither anterior instrumentation nor fusion were needed to maintain the stability and structure of the thoracic spine; 5) no destruction of posterior spinal elements; and 6) the patients returned to daily life sooner after the operation7,13).
This technique also had some disadvantages: 1) this method was technically demanding; 2) it is only indicated for beak-type OPLL at one or two consecutive levels; and 3) it is indicated only for the middle and lower thoracic spine9).
By this method, it could be possible to remove the OPLL via a wide field of view with minimal destruction, higher safety, and less blood loss. During removal of OPLL with the dura in view, operative safety could be possible. The favorable therapeutic effects were confirmed by 2-year follow-up after the operation. Despite the limited indications, this technique can be performed in the middle and lower thoracic spine and is particularly suitable for massive beak-type thoracic OPLL.
CONCLUSION
This surgical technique allows the surgeon to safely and effectively perform minimally invasive anterior decompression without instrumented fusion via a transthoracic approach for thoracic OPLL. It can be applied at the mid and lower level of the thoracic spine and could become a standard procedure for treatment of huge beak-type thoracic OPLL.